7 Ways to Improve Change Management in Healthcare

6 Mins
Updated: January 9, 2025
Published: February 13, 2024

Change leaders in healthcare face significant pressure today with the volume and pace of changes taking place in hospitals, clinics and other healthcare settings. To manage the tension between day-to-day realities and setting up teams for long-term success, you need to make change management more concrete for people on the front lines of the organization.
Improve Your Approach to
Change Management in Healthcare
These tactics and concepts can help you make change management in healthcare more understandable, doable and worthwhile to employee teams.
1. Enable leaders for their sponsor roles more thoughtfully
Leaders experience great pressure today just on the pace of work in healthcare. When equipping them to execute their sponsorship role, we need to do it in a way that feels manageable and worthwhile without feeling like we’re piling more onto their full plates. If we embed conversations about change management in already scheduled meetings, leaders not only follow through on activities, change management becomes an expected part of their work.
For one organization, a large steering committee and group of executive sponsors had been meeting on a regular basis to receive project updates and offer guidance to the project team. The change practitioner brought change management into the conversation by starting each meeting with 15 minutes to “flip the script,” asking sponsors to describe what they’re hearing from their teams when talking about the change.
Facilitating this activity each time the group met helped to set the expectation that sponsors would be talking to their teams regularly and reporting what they’re hearing back to their peers. This helped them build a new habit, which they continue to practice. It also provided insights for the change management teams about where they needed to improve communications or clarify aspects of the change.
2. Improve the employee experience to drive engagement and retention
In healthcare, the client or patient naturally comes first. But as employers, we need to look at this a bit differently and put our employees first. They need to feel valued and cared for if they’re going to bring their best selves to work and provide quality healthcare.
Focusing on the employee experience enables us to build desire for important and sometimes difficult changes throughout the organization. But the way an organization manages change overall improves the employee experience, which also helps address retention issues that healthcare organizations everywhere are experiencing today.
This starts with ensuring two-way communications between managers and teams during changes. As you help people move through their ADKAR journeys, you can remove barriers by having these conversations one-on-one or in groups to make sure you understand their concerns and ensure that they truly feel heard. For many change leaders, this will require a shift in the way you think about managing resistance to change. Instead of viewing resistance behaviors as people being difficult, you need to reframe resistance and come from a place of empathy and view it as an opportunity to solve a problem.
We also elevate the employee experience (and retention) by engaging people in shaping the direction of the changes that impact them and their daily work. Focusing on these activities increases employee involvement, helps people feel invested in the change, and reinforces their commitment to healthcare and your organization.
3. Address change fatigue and saturation
It’s not just healthcare leaders and sponsors of change who feel overloaded and fatigued by too many changes. Change saturation is mounting across the healthcare industry, and it’s having a significant impact on front-line employees. This is where taking an enterprise focus helps.
An enterprise focus creates intersections that aren’t visible in project-only change management. It develops in-depth knowledge about changes and enables you to see how each of the changes in your portfolio intersect, overlap and even collide. Building change capability in your organization can start many ways. An informal starting point is to create that space, so you start to see the big picture.
Learn how an academic health system successfully integrated two healthcare organizations,
deployed an ERP system, and developed change management as a leadership competency—all in a short timeframe—by deploying an effective ECM strategy.
4. Build employee conversations about change competency into everyday work
Understanding the importance of time is critical when dealing with healthcare staff who must embrace change. Their days are already packed to the brim with client and patient care while ensuring safety. There is never enough time to do all that needs to be done, let alone make time to try to improve approaches by working differently. But there is energy for change in healthcare because inefficient day-to-day approaches contribute to the problem. We need to be deliberate about solving for this dilemma by connecting changes and change competency to everyday work.
To be clear, it's not an “either or.” There isn’t time in the day to say, “Today, I'm going to focus on addressing these urgent issues, and then I'm going to switch gears to talk about change.” We need to integrate the two concretely. For example, during regular team huddles, one change practitioner asks team members, “What are you doing that is contributing to our desired future state? What are you doing that is moving us further away?”
Sometimes, you do need dedicated time to talk about bigger changes, like when you are preparing for an enterprise resource planning (ERP) or electronic medical record (EMR) system implementation. But more often, changes are small and easy to work into ordinary activities. The key is to think about ways of doing your work differently such that it becomes ingrained in work you have to do anyway. Those little things add up to something tangible. And this really helps set the groundwork for how you make big, meaningful and sustained changes take place.
5. Connect change to purpose
There is a powerful connection to purpose in healthcare. It doesn't matter where you work—back office, front office, patient-facing care—that commitment resonates everywhere. So, every time you talk about change, making the connection to purpose is critical. When an executive sponsor or manager communicates about a change, employees immediately think, “What are you talking about, and how is it going to make it better for me to do my job for my patients?” If you don’t have that message, it's as though they can't even hear you.
For leaders, this might mean speaking to improving client and patient outcomes, and the employee experience, during a town hall meeting. For managers, you can use standing team huddles and regular updates to webpages and intranet sites to connect the change to your purpose.
For example, one healthcare organization wanted to tackle incidences of incivility. The pandemic caused so much stress in the organization that they needed to regain focus on their core value of respect. Leaning in with managers and teams, change leaders facilitated the discovery process to help identify the issues they were facing, including the team members from the onset to build the culture of team collaboration.
Together, they identified how to use the tools, training and resources to address opportunities and make a difference. It was a shoulder-to-shoulder approach with managers as they engaged their teams. The work was intensive, but it enabled managers to elevate team dynamics and culture within their respective teams.

6. Build a change agent network
With any enterprise-wide change or strategy, you need help to deploy it locally. Building a network of change agents or ambassadors can help you advocate for and deploy the changes in different hospitals, offices, geographic regions, etc. Leveraging key influencers as change champions can also help busy managers fulfill their key roles during change.
Time between engagement and delivery is critical in change management. And, as mentioned above, the more you can engage people in building and designing solutions, the more they feel they have some control over how the change will affect them.
You can build a network of change agents to help your healthcare organization:
- Speed up deployment of healthcare system-wide changes
- Maximize people and resources to extend the scope and reach of changes
- Improve the flow of communication across a hospital or healthcare system
- Align change objectives at all organizational levels
- Develop change management skills in people in various roles across the organization
- Build credibility and trust for change management, especially when past changes have failed
- Enhance employee engagement and Desire to participate
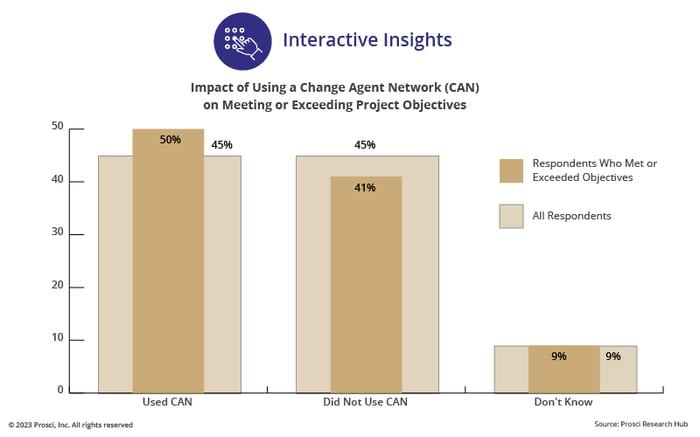
Prosci Best Practices in Change Management – 12th Edition research revealed that organizations that deployed change agent networks met or exceeded objectives more often than those that did not.
7. Make change management part of the way healthcare is done
Organizations should not think of change only in terms of projects or initiatives—change is integral to the nature of healthcare now. People are working on multiple initiatives at once. People need to come together to engage and leverage each other’s insights and connect to a broader purpose and the overall direction of the organization. This means building change capabilities throughout the organization through an effective enterprise change management (ECM) strategy.
ECM is about building capabilities and competencies in people at every level of your organization to more effectively bring about the many changes being introduced in your organization each year. As change management practices become institutionalized and embedded, each change the organization takes on is more successful, and your change management practice overall improves.
Manage Change Effectively in Healthcare
Change leaders in healthcare face immense pressures. By implementing strategic and concrete approaches to change management, you can navigate the tension between day-to-day realities and long-term success for your teams. From better enabling sponsors and building communication into everyday work to connecting change to purpose and building change capabilities in your teams, you can start to improve the way you manage change in healthcare and lead your team to greater success.



